Stroke
introduction
Stroke is the fourth leading cause of death in the United States, and the number one cause of disability in adults. Each year, approximately 795,000 people in the U.S. have a stroke, which means that someone has a stroke approximately every 40 seconds. Besides being one of the most common and most potentially devastating neurologic diseases, stroke is one of the most active areas of medical imaging research and innovation. Neuroradiologists can now look inside the brains of stroke patients and offer revolutionary treatments using advanced techniques that were unavailable even just a few years ago. The American Society of Neuroradiology is committed to supporting continuing research on stroke imaging, to ensuring that neuroradiologists provide the finest and most up-to-date care for their patients with stroke, and to helping patients, their families, and the general public learn more about stroke and the neuroimaging techniques that are used in the diagnosis and treatment of stroke. The following are some of the questions that people ask most frequently about stroke.
What is stroke? What is a transient ischemic attack?
A stroke occurs when part of the brain is permanently damaged, because it is deprived of the oxygen and nutrients it requires to function properly. Strokes are classified as either ischemic or hemorrhagic. In ischemic stroke, an artery in the brain is suddenly blocked and blood cannot flow to where it is needed. This kind of stroke is sometimes called a “brain attack,” because of its similarity to a heart attack, in which the blocked artery is in the heart rather than the brain. In contrast, in hemorrhagic stroke, a blood vessel in the brain ruptures and bleeds, which damages the surrounding brain cells. Ischemic strokes are much more common, accounting for approximately 87% of strokes. Most strokes occur in older adults, but people of all ages, even children, can suffer from stroke.
A transient ischemic attack (TIA) occurs when part of the brain is deprived of blood flow because an artery is blocked, causing symptoms like those of an ischemic stroke. However, in a TIA, the artery soon opens spontaneously, restoring blood flow. TIAs are sometimes called “mini-strokes.” However, unlike true strokes, TIAs are only temporary events, and the symptoms disappear when the artery opens. This generally occurs within a day, and often in less than an hour. Even though people who have TIAs feel better after the TIA is over, these people are at much greater risk of suffering from a true stroke that causes permanent brain injury, especially within the first few days following the TIA. For this reason, TIA should be considered a medical emergency, like stroke, and it is important to seek immediate medical attention if you think you have experienced a TIA.
Stroke and COVID-19
According to the Society of NeuroInterventional Surgery (SNIS), stroke surgeons are warning Americans that not calling 911 for help immediately if they see or are experiencing signs of stroke could be deadly. Ignoring stroke symptoms out of fear of overreacting or risking exposure to COVID-19 does not reduce the time-sensitive and potentially disabling and deadly nature of a stroke.
What are the risk factors for stroke? How can stroke be prevented?
Researchers have identified many risk factors for stroke. Unfortunately, some of these are simply unavoidable for people who have them. These uncontrollable risk factors include the following:
Age. Stroke is much more common in the elderly. The risk of stroke approximately doubles for every ten years of life after age 55.
Sex. Stroke is more common in men than in women. However, many women do suffer from stroke, and it is more common for women to die from stroke than men.
Race. Stroke is more common in African-Americans than in Americans of other races. This is probably at least in part because African-Americans are more likely to suffer from diabetes, high blood pressure, or obesity.
Family history. You are more likely to have a stroke if a close relative has had a stroke, particularly at an early age.
Prior stroke. If you have already had a stroke, your risk of having another stroke is greater than that of someone else of the same age and sex. The same is true of TIAs; a person who has had a TIA has a nearly 10 times greater risk of having a stroke.
Prior heart attack. Some of the medical problems that lead to stroke are similar to those that cause heart attacks, and people who have had a heart attack are more likely than other people to have a stroke.
Fortunately, there are many stroke risk factors that are controllable. You can reduce your risk of having a stroke by working to eliminate these risk factors from your life.
Controllable risk factors include the following:
High blood pressure. High blood pressure is the most important preventable risk factor for stroke. Americans are getting better at having their blood pressure checked regularly, and taking medication to treat high blood pressure when they need to. This may be a major reason why stroke has recently dropped from the number three cause of death in the U.S. to number four.
Smoking. Stroke is one of the many serious health problems that are caused by smoking.
Diabetes mellitus. People with diabetes have a higher risk of stroke than other people. If you have diabetes, you can reduce the risk of stroke by keeping you blood sugar under good control.
High cholesterol. A simple blood test can determine if the levels of cholesterol in your blood are higher than they should be. If this is the case, you can lower your cholesterol by choosing a healthier diet and exercising more, or, if your doctor recommends it, taking medications that lower blood cholesterol.
Physical inactivity and obesity. Regular exercise is important for maintaining a healthy weight, and reducing the likelihood of atherosclerotic disease, which can lead to stroke.
Atrial fibrillation. This is the most common cause of irregular heartbeat. In atrial fibrillation, the two upper chambers of the heart have a rippling motion, rather than contracting and emptying properly. This can allow blood clots to form within them, and these clots can then travel to the brain and cause an ischemic stroke. People with atrial fibrillation are up to seven times more likely to have a stroke. For some people with atrial fibrillation, doctors are able to restore the heart to its normal rhythm. When that isn’t possible, doctors may prescribe blood thinning medications that prevent blood clots from forming in the heart, thereby reducing the risk of stroke.
Carotid artery narrowing. The carotid arteries are arteries in the neck that carry blood to the brain. When they are narrowed because of atherosclerosis, this increases the risk that clots can form in them, and travel up to the brain, where they can cause an ischemic stroke. Carotid artery narrowing can be prevented by eating a healthy diet, exercising regularly, and, if necessary, controlling high blood pressure, high cholesterol, and diabetes. For some people whose carotid arteries are abnormally narrowed, doctors may prescribe blood thinning medications to prevent clots from forming in the carotid arteries. There are also surgical procedures that can be performed to reopen narrowed carotid arteries.
What are the symptoms of a stroke?
The symptoms of stroke vary widely, depending on what part of the brain is affected, and whether the stroke is ischemic or hemorrhagic. Some the most common symptoms are listed below. If you or someone around you experiences any of these symptoms, call 911 or your local Emergency Medical Services phone number to get immediate medical assistance. If possible, try to ascertain the time when the symptoms began, as this information can be extremely important in guiding stroke treatment once the patient has reached the hospital. Common symptoms are:
- Sudden numbness or weakness of the face, arm or leg, especially on one side of the body.
- Sudden confusion, or trouble speaking or understanding.
- Sudden trouble seeing in one or both eyes.
- Sudden trouble walking, dizziness, or loss of balance or coordination.
- Sudden severe headache with no known cause.
- [Source: American Stroke Association]
What treatments are available for stroke?
For patients with ischemic stroke, some of the most dramatic improvements are achieved by treatment with a drug called tissue plasminogen activator, or TPA. TPA is a “clot-busting” drug that dissolves blood clots, such as the ones that cause ischemic stroke by blocking arteries in the brain. TPA is injected intravenously (IV), directly into the bloodstream. It can be given only in a hospital, where doctors must perform certain important tests prior to its administration. If administered promptly, TPA can restore blood flow to the affected of the brain, thereby significantly reducing the effects of the stroke, and reducing long-term disability. However, IV TPA can only be used within three hours of the onset of stroke symptoms, or in some cases within four-and-a-half hours. Therefore it is extremely important to call for an ambulance immediately when someone first shows signs of stroke, and to try to note the time when symptoms began, if this is possible. Tragically, fewer than ten percent of stroke patients currently receive IV TPA treatment.
In some hospitals, blood clots that cause ischemic stroke can be removed by a more complex kind of treatment, in which a specially trained physician maneuvers a long, thin tube called a catheter into the blocked artery in the brain, and then uses devices or TPA delivered by the catheter to re-open the artery. This type of procedure, called endovascular therapy, requires highly trained personnel and specialized equipment. It is available only at relatively few hospitals, many of which are large medical centers. Like IV TPA, endovascular treatment must be initiated very soon after the onset of stroke symptoms. The time window is longer than for intravenous treatment, up to 8 hours from stroke onset. It can be performed either instead of or in addition to giving TPA. It is common for a stroke patient to be brought first to a local hospital where TPA can be administered quickly, and then transferred to a larger hospital where endovascular treatment can be offered if it is deemed appropriate. Endovascular therapy for ischemic stroke is discussed in greater detail below.
The treatments for hemorrhagic stroke are different from those for ischemic stroke. In hemorrhagic stroke, the main goals of treatment are to stop the bleeding, and/or to limit its effects upon the brain. Stopping the bleeding can be achieved in various different ways, depending on what the cause of the bleeding is. In many cases, bleeding in the brain is caused by an aneurysm, a small balloon-like outpouching that protrudes from one of the arteries in the brain. Aneurysms occur when there is a weakness in one part of the wall of the artery, causing that part to bulge outward. Many aneurysms are tiny, and remain present for many years without causing any problems. However, aneurysms can also grow over time, and the larger they are, the more likely they are to rupture. When an aneurysm ruptures, this typically causes sudden onset of a very severe headache, sometimes called a “thunderclap” headache, with or without other symptoms. Rupture of an aneurysm is an extremely dangerous event, and requires immediate treatment. In some cases, a neurosurgeon stops the bleeding by clipping the base of the aneurysm, using a small clamp-like device. Aneurysms can also be treated using endovascular procedures that are somewhat similar to those that are used for ischemic stroke. Hemorrhagic stroke can also be caused by other, less common kinds of treatable artery lesions, such as arteriovenous malformations (AVMs). Like aneurysms, many of these can be treated either with conventional surgery, or endovascular procedures.
What is a neuroradiologist, and how are neuroradiologists involved in the diagnosis and treatment of stroke?
Neuroradiology is a branch of the medical specialty of radiology. Radiologists are physicians who diagnose and treat disease by looking inside of the human body, using imaging techniques like x-ray, computed tomography (CT) scans, magnetic resonance imaging (MRI), and ultrasound. In the United States, radiologists receive four years of full-time specialty training in radiology after they have completed medical school. Neuroradiologists are radiologists who have undergone at least one, and sometimes up to three years of additional subspecialty training in the diagnosis and treatment of diseases of the brain and spinal cord, including stroke.
Computed Tomography (CT) Scans
When a patient arrives in a hospital’s emergency room with symptoms that suggest possible stroke, imaging tests are critical in making the correct diagnosis and enabling immediate treatment. Usually the first imaging test for such a patient is a CT scan of the head. A CT scan is performed using x-rays, such as those that are commonly used to detect a broken bone. However, a CT scanner uses x-rays in a more advanced way, in order to produce cross-sectional images that look like “slices” of the brain, or three-dimensional images.
CT scans are excellent at detecting the bleeding in the brain that occurs in hemorrhagic stroke. However, ischemic stroke may be difficult or impossible to see in CT images, especially during the first few hours after the stroke occurs, which is the period when treatment decisions are most important. Therefore, if doctors strongly suspect that a patient is having a stroke, they will often give the patient IV TPA even if the CT scan does not show an ischemic stroke, provided that the scan also does not show a hemorrhagic stroke. Giving TPA to a patient with a hemorrhagic stroke would be very dangerous.
Often, after first obtaining a CT scan of the head in the usual way, the scan will be repeated during an intravenous injection of a type of dye called a contrast agent. This technique is called CT angiography, or CTA. Neuroradiologists can use CTA to produce sophisticated 3D images of the blood vessels inside of the brain, which otherwise are not visible in CT images. In patients with ischemic stroke, neuroradiologists use CTA images to identify which blood vessels are blocked, and this information can be helpful in deciding how to treat the patient. In hemorrhagic stroke, CTA often shows the aneurysm, arteriovenous malformation, or another kind of blood vessel problem that is responsible for the bleeding. In hemorrhagic stroke, finding the source of the bleeding is often the most important first step in making the bleeding stop.
In many hospitals, patients who are suspected of having an ischemic stroke also undergo a third type of CT scan, called CT perfusion imaging, or CTP. CTP involves a second injection of the same contrast agent that is used for CTA. Unlike CTA, which creates pictures of the large arteries that bring blood to different regions of the brain, CTP measures the flow of blood through the microscopic blood vessels that are small enough for the brain to extract oxygen and other nutrients from them. Neuroradiologists can use CTP to measure a variety of different aspects of this process, such as the overall amount of blood that is flowing through a particular part of brain, or the speed with which the blood is flowing. This information can be used to make decisions about how best to treat ischemic stroke patients.
CTA and CTP are performed using the same type of scanner that is used to produce conventional CT images, and the various kinds of images are usually obtained together, as part of the same examination. Adding CTA or CTP lengthens the examination by several minutes. Patients undergoing CTA or CTP often experience a transient sensation of warmth or tingling while the contrast agent is being injected into them, but most people do not experience this sensation as unpleasant, and it disappears after just a few seconds. Whereas any patient can have a conventional head CT examination, there are some patients who cannot safely receive the intravenous dye that is required for CTA or CTP, either because they are allergic to it, or because a blood test shows that their kidneys are not functioning well. In patients with poor kidney function, injection of the dye could cause further kidney injury.
Magnetic Resonance Imaging (MRI)
MRI, like CT, is an advanced medical imaging technique that can produce slice-like or 3D images of the brain. However, MRI scanners and CT scanners work in very different ways. MRI scanners produce images using not x-rays, but instead a combination of extremely powerful magnets, which are more than 20,000 times as strong as the Earth’s magnetic field, and radio waves, similar to those that are used to transmit sounds through the air. MRI scanners are controlled by highly sophisticated computer programs, which can be designed to produce many different kinds of images, showing different aspects of the brain and its functioning. Neuroradiologists can customize each patient’s brain MRI examination, so as to produce a combination of different types of images that individually address his or her particular medical problem.
For stroke patients, one of the most important kinds of brain MRI is diffusion-weighted imaging, or DWI. Unlike other medical imaging tests, DWI can measure the speed at which water molecules self-diffuse, or move randomly, in different parts of the brain. This diffusion process slows down greatly in parts of the brain affected by ischemic stroke. Therefore, DWI can detect ischemic stroke within mere minutes of stroke onset, a time when other imaging tests show no apparent abnormality.
Other types of MRI images can show different kinds of problems in the brain. For example, MRI scanners can be programmed to show the bleeding that occurs in hemorrhagic stroke. It is also possible to use MRI to study the blood vessels in the brain, using magnetic resonance angiography (MRA), a technique that produces images similar to those obtained with CTA. Another MRI technique, called MR perfusion imaging (MRP) or perfusion-weighted imaging (PWI), is like CTP, in that it allows neuroradiologists to obtain different kinds of measurements of the flow of blood through different parts of the brain.
What is an interventional neuroradiologist, and what special treatments can they offer?
Endovascular or intra-arterial treatment of ischemic stroke
Patients who are suffering from a severe ischemic stroke due to the blockage of a large brain artery may be candidates for catheter-based treatment to open up the vessel. This type of treatment is performed under real-time x-ray imaging which is controlled by the interventional neuroradiologist. As mentioned above, this type of imaging requires dedicated equipment, which is housed in a special interventional neuroradiology suite. These suites resemble operating rooms, in that great care is taken to maintain a sterile environment within them.
Patients undergoing interventional neuroradiology procedures are given anesthetic agents to minimize their discomfort. Depending upon the procedure, these anesthetics may range from injection of a small quantity of local anesthetic to general anesthesia, like that used in major surgical procedures.
Most interventional neuroradiology procedures begin with insertion of a catheter into the femoral artery, which is a large artery located in the groin. The catheter, which is a long, flexible hollow tube, is threaded over a guide wire up into the aorta, the main artery supplying the body, and then into the neck vessel leading to the blocked brain artery. Images of the artery (also known as angiography) are then taken using a radiographic contrast dye similar to the one used for CT angiography. These pictures allow the interventional neuroradiologist to identify the site of occlusion and plan the intervention. A smaller catheter (microcatheter) is then placed through the initial catheter and past the occlusive clot.
There are two main approaches to clot removal: whole-clot retrieval (or thrombectomy) and clot aspiration. In the first technique, the clot retrieval device is placed through the microcatheter, and opened across the clot. The device which traps the clot is then removed. The second technique, clot aspiration, involves fragmentation and suction of the clot. This is performed using catheters larger than traditional microcatheters, which provide increased suction power. Thrombectomy and aspiration techniques are often used in combination. In addition to these mechanical approaches, many interventional neuroradiologists also use local TPA infusion into the clot to help dissolve it.
Endovascular treatment for acute stroke is more successful than intravenous TPA alone in opening blocked blood arteries. Rapid opening of arteries is, in turn, associated with an improved chance of a meaningful recovery. However, not all patients with ischemic stroke are candidates for endovascular treatment. In order for endovascular treatment to be considered, neuroradiologists must identify a blocked artery that is large enough to allow access with a catheter. There are also risks associated with endovascular treatment, the most important of which include bleeding into brain tissue that has already died, occlusion of previously uninvolved arteries (i.e., new strokes) and vessel injury.
Endovascular treatment of hemorrhagic stroke
Aneurysms are the most common treatable vascular lesions that cause hemorrhagic stroke. When a bleeding aneurysm is discovered, closing the ruptured aneurysm and stopping the bleeding quickly is imperative, in order to prevent early re-rupture, which is associated with high rates of death or severe disability. Traditionally, bleeding aneurysms were closed by neurosurgeons, who can open the skull and attach a small clip directly to the aneurysm. This technique is still preferred in some circumstances, depending upon the condition of the patient and the characteristics of the aneurysm. However, recent therapeutic innovations now allow interventional neuroradiologists to treat aneurysms without open surgery, using a procedure called endovascular coiling.
Like endovascular treatment of ischemic stroke, which has been described above, endovascular coiling usually begins with insertion of a catheter into the femoral artery, and advancement of the catheter into the arteries of the brain. The catheter is carefully maneuvered into the aneurysm, using real-time x-ray image guidance. Once the catheter is in place, an even smaller microcatheter is carefully placed through the initial catheter into the aneurysm. Tiny flexible platinum coils are then delivered through the microcatheter into the aneurysm, and, detached, once their proper positioning have been confirmed. Coils are sequentially deposited, one after another, until the aneurysm has been successfully closed. In some cases, a small balloon is temporarily inflated at the opening of the aneurysm, in order to make sure that no coils slip out during placement. Rarely, holding the coils in place requires placement of a permanent stent, which is a hollow tube that can be used to block the opening of the aneurysm until it heals. All of these procedures are performed via the catheter, and no open surgery is required. Long-term follow up imaging is required to assess the durability of the coiling procedure. In approximately 20% of cases, the aneurysm may reopen partially. Up to half of these reopened aneurysms may require retreatment.
During the first two weeks after aneurysm rupture, approximately 20% of patients are at risk for ischemic stroke because their bleeding causes vasospasm, in which spasms of the blood vessels in the brain cause them to narrow severely.Vasospasm often may be treated successfully using intravenous medications. However, if this fails to improve the patient’s symptoms, endovascular treatment may be necessary. In endovascular treatment of vasospasm, an interventional neuroradiologist advances a catheter into the narrowed artery, and either delivers a vessel-relaxing drug directly into it, in order to relieve the spasm, or gently inflates a small balloon, which dilates the vessel and helps to restore normal blood flow.
Arteriovenous malformations (AVMs) are less common vascular lesions that may also cause bleeding in and around the brain. An AVM consists of a tangled network of abnormal blood vessels that are fragile, and prone to rupture and bleeding. Interventional neuroradiologists use catheters to treat AVMs in a variety of different ways, in order to stop or prevent their bleeding. For example, aneurysms that develop within an AVM can be filled with coils, as described above. Also, the AVM, or the vessels that supply it with blood, can be intentionally blocked with a glue-like substance that is delivered by a catheter. Because every AVM is different, an individual patient’s treatment options may include several different endovascular techniques, and/or other kinds of treatment that are performed by physicians other than neuroradiologists. For example, radiation oncologists can treat AVMs with radiation to make them shrink, and neurosurgeons can surgically remove part or all of an AVM.
NEURORADIOLOGY IMAGES
The following images, all obtained from a single patient, are examples of the different kinds of techniques that neuroradiologists may use in the diagnosis and treatment of stroke. This patient was a 63-year-old man who came to a hospital emergency department several hours after the sudden onset of very severe symptoms, including inability to move one side of his body
 .
.
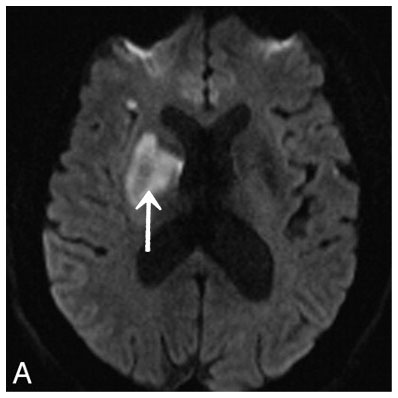
Image A: This is a kind of brain MRI image called a diffusion-weighted image (DWI). The white lesion (shown by arrow) is an infarct, a part of the brain that has died because it has been deprived of blood flow. In this case, the patient recognized the symptoms of stroke and came to the hospital immediately, and therefore the infarct is still relatively small.
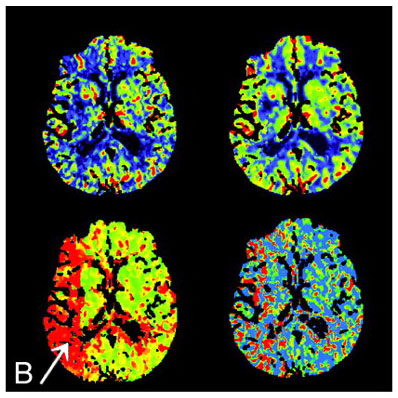
Image B: These are perfusion images, which a neuroradiologist can use to study the flow of blood to different parts of the brain. The arrow indicates a part of the brain where the blood supply is impaired. The region of abnormal blood supply is much larger than the region that is already dead (Image A). If the problem is not fixed immediately, some or all of this additional brain tissue may die as well, making the patient’s symptoms permanent, and possibly resulting in life-threatening complications.
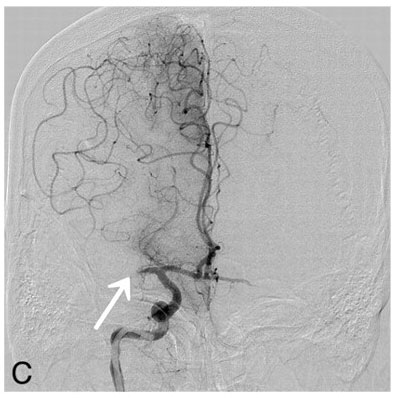
Image C: This image is an angiogram, obtained by an interventional neuroradiologist at the beginning of an endovascular treatment procedure. The dark structures are arteries, which have been made visible by injection of contrast dye through a long catheter that has been advanced from the patient’s groin into an artery in the head. The artery identified by the arrow is blocked by a blood clot, which is responsible for the infarct seen in Image A, and the large region of impaired blood flow seen in Image B. After seeing this image, the interventional neuroradiologist began trying to remove the clot and restore blood flow.
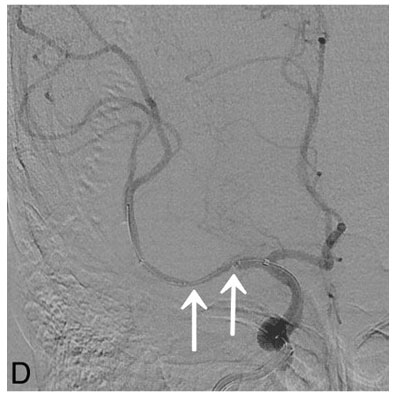
Image D: This angiogram was obtained after the interventional neuroradiologist inserted a stent, a tube-like device that is used to hold a blood vessel open. The artery is no longer blocked, but there are still two points where it is abnormally narrowed (shown by the arrows).
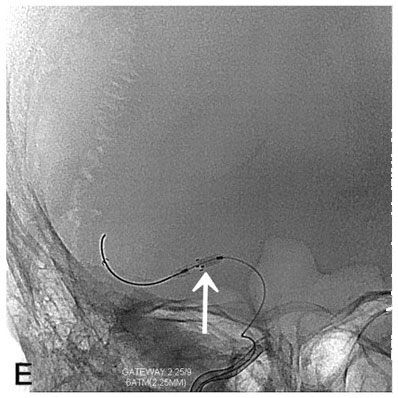
Image E: This simple x-ray image was obtained during the endovascular procedure, without injecting additional contrast die. The arrow points to a small balloon that has been inserted by the interventional neuroradiologist, and inflated within the narrowed blood vessel, in order to open it further. This part of the procedure is called angioplasty.
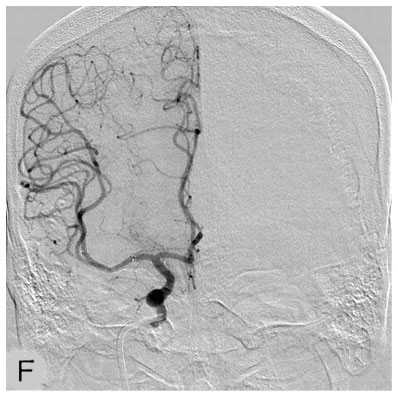
Image F: This angiogram, performed following angioplasty, shows that the artery is no longer narrowed. The patient’s condition improved dramatically after the procedure, and he was able to leave the hospital with only minimal symptoms that did not impair his quality of life significantly.
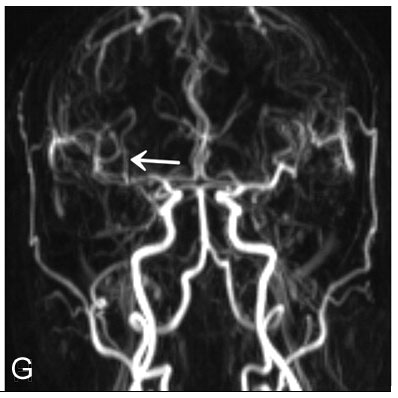
Image G: Nine days after his stroke, the patient had a follow-up MRI examination, which included this magnetic resonance angiogram (MRA) image. This image, which did not require the use of an arterial catheter or any contrast dye, shows that the artery that was reopened by the endovascular procedure has remained open.