Alzheimer's Disease
Introduction: The Impact of Alzheimer's
Alzheimer's disease is the most common form of dementia in older patients. Although much has been learned about the disease over recent years, its underlying cause remains unknown. The disease currently affects millions of people worldwide, and is becoming increasingly prevalent as the population ages and as lifespans become longer. Some have suggested that the number of individuals affected by Alzheimer's could quadruple over the next 50 years. This dismal scenario suggests that the enormous financial and social burden of Alzheimer's disease will continue to grow. However, if it were possible to improve our ability to determine which patients are at risk of developing the disease, to recognize early forms of the disease and to start treatment immediately, and to monitor the effects of treatment, we could substantially brighten our future. Indeed, a modest goal of delaying disease onset by just two years would result in 2 million fewer cases of Alzheimer's disease by the year 2050.The past two decades have witnessed rapid advances in the use of imaging techniques for evaluating disease processes in the living human brain. Particularly in the case of Alzheimer's disease, a definitive diagnosis could not be previously be obtained until after the patient had died. However, powerful new tools for imaging the brain's structure and function have been developed and and contribute important information to establish the diagnosis before death and to define prognosis in the individual patient. Imaging is also likely to play an increasing role in evaluating the effectiveness of new medications that are being designed to delay the onset or slow the progression of Alzheimer's disease. Two especially valuable imaging techniques currently available are magnetic resonance imaging (MRI) and positron emission tomography (PET).
MRI Evaluation of Alzheimer's
MRI works by using a powerful magnet to create highly detailed pictures of brain anatomy. Applied differently to focus on function instead of anatomy, it can also be applied to evaluate how the brain responds to thinking or movement tasks. Importantly, brain MRI is obtained in many patients to ensure that another problem such as a brain tumor is not responsible for a patient’s symptoms. Furthermore, the brain slowly shrinks with aging in all people, but this process is accelerated in patients with Alzheimer's disease. The shrinkage also has a different regional variation across the brain in patients with Alzheimer’s compared to healthy elders. The hippocampus, an area of the brain that controls memory, is particularly affected in Alzheimer’s. Shrinkage of the hippocampus may be detected with MRI early in the course of Alzheimer's dementia, and this finding can be used to support a clinical diagnosis of Alzheimer’s. However, this is a late finding in the overall disease process, and techniques aimed at evaluating brain function (or how the brain responds to stimuli) tend to be even more sensitive for detecting the disease at its very earliest stages. An advantage of MRI is that it does not use ionizing radiation. However, people who are uncomfortable in small spaces (those with claustrophobia) may sometimes find it difficult to undergo MRI. Also, those with a history of having certain kinds of metal in their body, such as a pacemaker or an internal ear implant, may be unable to undergo MRI.PET Evaluation of Alzheimer's
PET imaging provides physicians with the means to examine how the brain uses sugar (glucose) for energy. Because this form of energy drives all brain processes including cognition, PET provides a picture of brain metabolic function. PET works with the injection of a tiny amount of a radioactive drug through a small plastic tube in the patient's hand or arm. (The amount of radiation received is comparable or less than that of many medical imaging tests such as a computed tomography [CT] or a stress test.) The PET scanner then takes a series of pictures of the brain, following the drug as it courses through the patient and ultimately collects within the neurons in the gray matter of the brain.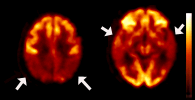 |
| Fluorodeoxyglucose (FDG) PET images demonstrated diminished sugar (glucose) use by the brain in the parietal (left) and temporal (right) regions (arrows) of the brain. |
The imaging of brain energy metabolism with PET is an effective test for distinguishing Alzheimer's disease from other forms of dementia, such as frontotemporal dementia. Decreased metabolism in the temporal and parietal regions of the brain is typical and highly suggestive of Alzheimer's disease in a patient with memory changes. This pattern has also been observed in individuals with family members in whom Alzheimer's disease was diagnosed at a young age.
PET scanners have become much more widely available over the past few years, as PET is now also used for diagnosing cancers elsewhere in the body. Thus, PET imaging may be used more frequently in the future in the diagnosis of dementia. In fact, the Health Care Financing Administration (HCFA) is currently reviewing whether to approve Medicare reimbursement for clinical PET imaging in cases of suspected Alzheimer's disease.
Glucose is not the only substance that can be imaged with PET. With special drugs, other brain structures and metabolic processes can also be imaged with PET in brain areas thought to be involved in the development of dementia. One hallmark of Alzheimer's disease is the abnormal deposition of a protein called amyloid in the cellular space outside of neurons. This protein has previously been used to diagnose the disease after death, but can now be detected noninvasively using PET agents. One currently FDA-approved agent, florbetapir, and others under development can be used with PET to visualize the deposition of amyloid in the brain. Although the technique has yet to become widely used, amyloid imaging may be highly useful in the future for diagnosing Alzheimer's disease, for tracking the effects of treatment, or for establishing risk even before a person becomes aware of symptoms.